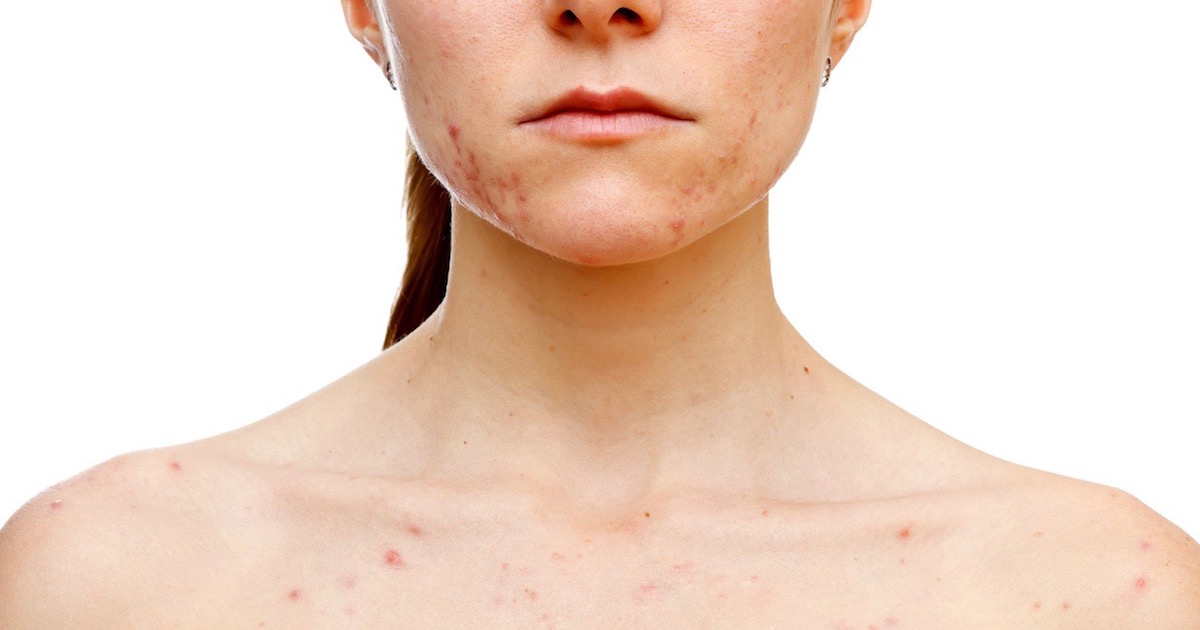
OCD and Skin Picking: Understanding Causes, Treatment Options, and Recovery Strategies
You might notice urges to pick your skin that feel automatic, soothing, or impossible to stop—and those urges can be part of a recognized condition called excoriation (skin-picking) disorder, which often overlaps with obsessive-compulsive disorder. If skin picking is causing damage or distress, it usually reflects a treatable condition that deserves attention rather than shame.
This article explores OCD and skin picking, helping you understand how obsessive thoughts and compulsive actions can drive skin picking, what biological and environmental factors commonly play a role, and which evidence based treatments clinicians use to reduce harm and regain control. Expect clear, practical information that shows why these behaviors happen and what steps you can take to find relief.
Understanding OCD and Skin Picking
You will learn how obsessive thoughts and repetitive behaviors connect, what skin picking looks like clinically, how the two conditions overlap, and which signs should prompt professional help.
Defining Obsessive-Compulsive Disorder
Obsessive-Compulsive Disorder (OCD) involves persistent unwanted thoughts (obsessions) and repetitive actions or mental rituals (compulsions) performed to reduce anxiety. You might experience intrusive fears—about contamination, harm, or symmetry—that feel irrational yet produce intense distress.
Compulsions can be visible (handwashing, checking) or mental (counting, repeating phrases). These behaviors often consume hours daily and impair work, school, or relationships. Effective treatments include cognitive-behavioral therapy with Exposure and Response Prevention (ERP) and, when appropriate, selective serotonin reuptake inhibitors (SSRIs).
What Is Skin Picking Disorder?
Skin Picking Disorder, or excoriation (dermatillomania), is a body-focused repetitive behavior where you repeatedly pick at skin causing damage. Picking targets can include pimples, scabs, or healthy skin and often leads to bleeding, scarring, or infections.
You may pick to reduce tension, to remove perceived imperfections, or automatically while distracted. Unlike simple habits, the behavior continues despite attempts to stop and creates significant distress or functional impairment. Habit Reversal Training (HRT) is a primary behavioral treatment, often combined with supportive psychotherapy.
Links Between OCD and Skin Picking
Skin picking and OCD share features: repetitive actions, difficulty resisting urges, and relief after performing the behavior. Neurobiological overlaps include differences in brain circuits that regulate habit formation and impulse control, and some people respond to similar medications like SSRIs.
However, not all skin picking is OCD-driven. You should note distinctions: OCD compulsions are typically linked to specific intrusive thoughts and driven by anxiety reduction, while excoriation can arise from sensory urges, boredom, or appearance concerns (as in Body Dysmorphic Disorder). Accurate diagnosis matters because treatment emphasis differs—ERP for classic OCD rituals, and HRT or tailored therapies for body-focused repetitive behaviors.
Recognizing Symptoms and Warning Signs
Watch for repeated skin picking that you cannot control and that leads to tissue damage such as sores, scabs, or scars. Note if picking consumes significant time each day, causes infections, or interferes with social and occupational functioning.
Other warning signs include attempts to conceal damage, picking during passive activities (watching TV, reading), or picking driven by intrusive thoughts about dirt or imperfections. If you experience suicidal thoughts, severe distress, or quick escalation of skin damage, seek urgent professional care.
Causes, Consequences, and Treatment Options
You will find why skin picking often starts, how it affects your body and mood, how clinicians evaluate it, and which treatments have the strongest evidence for help.
Underlying Psychological Factors
Skin picking often links to obsessive-compulsive patterns, anxiety, or emotional regulation difficulties. You may pick to reduce tension, respond to intrusive thoughts about perceived skin imperfections, or self-soothe during stress.
Impulsivity and sensory-seeking behavior can drive repetitive picking; some people report strong urges tied to specific textures or perceived irregularities.
Comorbid conditions—major depressive disorder, generalized anxiety disorder, or body-focused repetitive behavior disorders—raise both risk and severity.
Learning and reinforcement matter: temporary relief after picking reinforces the habit, making it more automatic over time. Habit-reversal components target these learned triggers and responses.
Physical and Emotional Effects
Repeated picking causes visible skin damage: scabs, open wounds, scars, pigment changes, and sometimes infection.
Infections can require antibiotics or wound care; severe scarring may need dermatologic treatments like laser therapy or surgical revision.
Emotionally, you may feel shame, embarrassment, or social withdrawal because of visible lesions. Those feelings can feed more picking, creating a cycle.
Work, relationships, and daily routines may suffer if picking consumes time or leads you to avoid social situations. Monitoring complications and documenting patterns helps clinicians tailor treatment.
Diagnosis and Assessment
Clinicians diagnose excoriation (skin-picking) disorder when picking is repetitive, causes tissue damage, and leads to marked distress or functional impairment.
Assessment includes a detailed history of frequency, triggers, and attempts to stop; the clinician checks for rule-outs such as dermatologic disease or substance use.
Standardized tools—like clinician interviews and self-report scales—measure severity and track progress. Photographs and lesion maps can document objective change over time.
Evaluate comorbid psychiatric conditions and medical risks (infections, scarring) because treatment planning depends on your full clinical picture.
Evidence-Based Treatment Approaches
Cognitive-behavioral therapies form the foundation of treatment, especially habit-reversal training (HRT) and stimulus control.
HRT teaches awareness of urges, competing responses (e.g., clenching fists), and strategies to change the environment that triggers picking.
Exposure and response prevention (ERP) and acceptance-based CBT address anxiety-driven picking and reduce the need to neutralize distressing thoughts.
Medications can help when symptoms are severe or when comorbid conditions exist: selective serotonin reuptake inhibitors (SSRIs) have evidence for some patients.
Dermatologic care treats wounds, infections, and scarring; combining skin care with behavioral treatment improves outcomes.
Consider multidisciplinary care—mental health, dermatology, and primary care—when you face persistent picking, infection risk, or significant psychosocial impact.
Keep an eye for more latest news & updates on Aiotechnical!